Historically, payers and providers have maintained ‘arm’s length relationships’ with each party acting in accordance with what they deemed their own best interest. Both parties were wont to hold on to data and processes each deemed proprietary to their business model. Or if shared might be harmful to their market position and operating margins. At worst, payers and providers may engage in antagonistic relationships and point fingers at each other when their members and patients complain. Nowadays with the increasing adoption of value-based payment models, mandates such as the Transparency in Coverage Rule and No Surprises Act, and the entry of non-traditional payers and service providers, it’s critical that payers and providers collaborate with each other, share information in ways beneficial to everyone involved, and recognize their mutual survival depends on using data and technologies to offer a fair service at a fair price in the most frictionless way possible.
Fair Service at a Fair Price in the Most Frictionless Way Possible
There are many considerations, challenges, and actions involved with defining what constitutes a fair service and a fair price – and several traditional and emerging points of friction between stakeholders that must be acknowledged and addressed. The No Surprises Act and the Information Blocking rule in the 21st Century Cures Act are examples of broad regulatory attempts aimed at reducing payer and provider friction with healthcare consumers and patients. Additionally, the increasing use of telehealth services, changes in CMS reimbursement for various settings including home health and skilled nursing facilities, and continuing growth in the use of high-cost drugs are just a few of the reasons for adopting payment integrity programs.
RELATED: Surprise Billing and the Impact for Payors
Payment Integrity: Balancing Cost Savings & Reducing Provider Abrasion
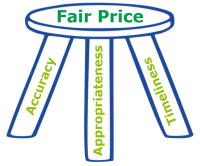
It should be no surprise that the amount paid for a specific healthcare service – or outcome in the case of value-based care – can be a key point of friction between payers and providers. Accuracy, appropriateness, and timeliness comprise individual legs of the three-legged stool of fair price. And each of these legs presents specific technical, clinical, and organizational challenges that payers and providers must understand and address – whether in a fee-for-service or value-based arrangement and whether paid retrospectively or prospectively.
To build a strong foundation supporting fair services at fair prices in the most frictionless way possible, payers and providers must balance the maximization of savings from payment integrity programs with minimizing provider abrasion.
RELATED: Trends that are re-shaping payment integrity strategies
Get Answers to Your Questions & Share Your Insight & Ideas
Our 1st Focus Area Roundtable on Payment Integri
- How can providers and payors find common ground in terms of setting prices and reimbursement?
- In what ways will the No Surprises Act change the future of provider networks?
- How must payment integrity programs evolve to ever be considered by providers as fair?
Join other healthcare leaders and changemakers on Thursday, September 9, 2021 at 11:00 AM PT / 2:00 PM ET for the first of a series of roundtables facilitated by our Focus Area Partner MultiPlan. Request your invitation today.