
In the session titled “How Technology Innovation Will Play a Critical Role in Prevention” at last week’s 2019 AHIP Consumer Experience & Digital Health Forum in Chicago, a gaggle of industry leaders, innovators and change-makers shared their thoughts and ideas on the critical role new innovations in technology will play in prevention (of accidents & disease) among the fastest-growing demographic—aging Boomers joining original Medicare and Medicare Advantage programs at the rate of 10,000 new beneficiaries a day.
Neel Mehta from Honor moderated a panel consisting of Bryan Adams of Best Buy Health, Dr. Ari Melmed, MD of Kaiser Permanente Colorado, Rajeev Ronanki from Anthem, and Faraz Shafiq of Cambia Health Solutions. The panel shared their take and experiences on the following:
- Latest innovations that can help keep older adults healthy and safe in their homes
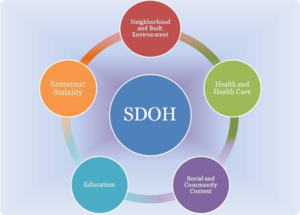
- The impact technology might have on the social determinants of health
- How these technology innovations can result in better outcomes for well-being
The remainder of this post shares a few highlights from the session. Access all recordings mentioned in this blog post here.
Highlights on How Technology Innovation Will Play a Critical Role in Prevention
The following are some of the questions that moderator Neel Mehta presented to the panel and some panelist responses to those questions. You can listen to the entire recording – admittedly not of the best quality but still enlightening – here. Specific starting and ending points in the recording are noted below and link to the audio recordings.
Q1: How do health plans support caregivers? (02:24 – 04:30)
Fariz Shafiq: On average, caregivers provide 32 hours a week of unpaid caregiving, essentially a full-time, unpaid job imposing a financial and emotional impact on the caregiver. As a health plan, we recognize that caregiving is an extremely important service. Fariz shared how his organization equips caregivers best:
- Help with scheduling appointments and checking the efficiency of patient schedules
- Reconciling medications
- Help with understanding and paying bills
Rajeev Ronacki: Keeping on top of local resources is a real challenge. We provide members and patients digital apps and help identify and connect members and patients with community-based orgs that can assist them. And we provide an online marketplace where members and patients can also self-serve.
Tech and Touch Must Be Balanced for Innovative Prevention of Accidents & Disease
Q2: The elderly caregiver population, whether it’s home care, provider or family member, are difficult to reach and engage with, regardless of whether they are tech-savvy or not. What are some of the ways you reach this population? (06:45-08:47)
Bryan Adams: Everything starts with balancing the tech vs. touch concept. We want to leverage technology into the home and surround that with robust services. This will ultimately move the needle not only for the healthcare consumer but also for the healthcare system as a whole.
We have ‘healthcare caring centers’ staffed by people encouraged and trained to have a high level of empathy interaction. Mostly telephonic relationships that establish and nurture a tech vs. touch relationship with the senior.
Q3: One of the things that is appealing to tech innovation in healthcare is Artificial Intelligence. What do you think in your perspective as a provider is the role of the healthcare provider in respect to AI? (08:53-12:53)
Dr. Ari Melmed: It’s a new time for providers and physicians. The role of the provider is to partner with the patient and to address their concerns. To get them the right answers. The amount of information available to everyone online is overwhelming. Staying up to date as a physician nowadays only takes 21 hours a day.
Faraz Shafiq: Computers are helping doctors getting better at diagnoses. Healthcare is so complex and the volume of information so great and often so nuanced that AI-powered assistance is needed. (10:42-12:09)
RELATED: How Cambia Health Solutions is Leveraging Artificial Intelligence in Healthcare Space
Using Technology & Data to Understand Social Determinants of Health
Q4: I have found that on the medical side there’s a mountain of data. And on the social side there’s a huge and growing amount of data. How can technology support the understanding of how social and community health factors influence outcomes? (13:10 – 15:00)
Rajeev Ronacki: I think the question is what do we do about it? How do we react to it? How do we make it more democratized?
Listen to more of Rajeev’s response here.
Q5: What are some of the challenges in integrating data, making it uniform, and making it ‘analyzable?’ (15:33-19:18)
Rajeev Ronacki: Roughly 80% of the work we need to do on any AI initiative is data prep: obtaining the data, looking at the quality of data, cleansing and integrating it, creating standards for uniformity. There’s nothing secret about it.
Listen to other responses to this question here.
Brick & Mortar Bring Human Interaction and Touch to Accident & Disease Prevention
Q6: What unique value do brick and mortar companies bring to healthcare? (20:20 – 23:20)
Bryan Adams: Brick and mortar locations enable the touch component of the critical need to balance technology and human touch/interaction mentioned before. This is particularly important for the senior population.
Being entrenched in the neighborhood and being involved with community care initiatives helps us to better understand and capture social determinants of health unique to that area and then take that information and make it actionable. At our company, we’re giving thought on how to leverage our Geek Squad (20,000 people) and over 1200 retail outlets to engage with health plan members and to advance preventive care.
Q7: If telehealth has not yet reached into the home it is gaining a footprint in places like Best Buy, Walmart, and Walgreens. Are you seeing brick and mortar playing a part in expanding the reach of telehealth? (23:40 – 25:20)
Dr. Ari Melmed: Yes. And there are different ways of thinking about telehealth like onsite work clinics which are playing an important role, schools are developing innovative programs, remote clinics are interfacing with centralized, specialized services.
Q8: How has the Medicare market shifted in trying to support senior’s health? (25:24 – 28:50)
Rajeev Ronacki: Increasingly there’s a consumer preference to do things in the home – particularly in the transition to and from the hospital.
Using TV’s and sensors and voice-assistance to deliver the care that’s needed. I would venture to say that 60-70% of the care that doesn’t need active intervention can be provided in the home. The question is how to deliver it in a way that makes sense.
Bryan Adams: Medicare Advantage as a whole has become a hub of innovation and we’re excited about SSBCI and opening up the ability to address social determinants. (27:31 – 28:38)
Can Technology Address 50% of Preventive Health Measures?
Q9: As Rajeev mentioned, with the right technology 60-70% of the care that doesn’t need active intervention can be provided in the home. What will it take to get to widespread adoption of the minimum technology infrastructure needed to address 50% of preventive medicine? (28:50 – 32:13)
Rajeev Ronacki: Some sort of super simple, USB-type device that’s widely adopted by consumers. Installation and implementation need to be simplified and cost-effective.
Listen here from more on how technology in the home may address 50% of preventative medicine.
Q10: Are there any examples of technologies that are starting to scratch the surface of being pretty easy to use? (33:35 – 38:50)
Rajeev Ronacki: Wireless sensors and other devices are becoming increasingly sophisticated and easy to use.
Bryan Adams: Passive devices that operate in the background and do not require the member/patient to do anything special or change any behavior. Devices that measure ADL’s and allow the member/patient to keep living their life without any special attention.
Dr. Ari Melmed: Devices that provide feedback on a real-time basis to drive behavior change. Tools to extract information from medical records and help the physician more quickly understand salient aspects of the patient.
Connect with Healthcare Industry Executives, Leaders, Innovators & Change-Makers
For more information, insight, and ideas on healthcare innovation and the transformation of healthcare, subscribe to our eNewsletter and consider becoming a member of the HealthCare Executive Group.








[…] the session titled “How Technology Innovation Will Play a Critical Role in Prevention” at last week’s 2019 AHIP Consumer Experience & Digital Health Forum in Chicago, a gaggle of […]